Last Updated December 20th, 2021
Overview of spondylitis
The current global burden of musculoskeletal diseases is extremely high. The World Health Organisation (WHO) estimates that around 50% of the current global population suffers from different types of musculoskeletal diseases. These diseases aggravate more to give rise to degenerative bone diseases. The most common disease belonging to this category is spondylitis. The scenario is quite grave in India. Nearly 0.25% of the Indian population suffers from spondylitis, mostly accompanied by spine stiffness. A particular form of this disease known as ankylosing spondylitis affects nearly 0.1-1.8% of people globally. The statistics of the Arthritis Foundation, United States show that around 350 million people in different parts of the world suffer from 140 different types of arthritis.
What is spondylitis?
 Spondylitis is defined as an inflammatory condition that affects the vertebra. It is a form of spondylopathy, which is a class of vertebral diseases, marked by pain, inflammation, and immobility of the spine and the adjoining, structures (ligaments and tendons). Spondylitis that involves multiple vertebral joints is known as spondylarthritis. In many cases, the sacroiliac joint, that connects the spine with the pelvis also becomes inflamed. Some of the neighboring joints such as that of the shoulders, ribs, knees, hips and often, the lower extremities are also affected. The places where the ligaments and the tendons attach to the bones also suffer inflammation. The patients typically experience mild to moderate back pain which is intermittent in nature. In the more advanced stages, a fusion of the affected bones occurs, leading to the loss of flexibility of the bones, stiffening of the rib cage and a subsequent reduction in lung capacity.
Spondylitis is defined as an inflammatory condition that affects the vertebra. It is a form of spondylopathy, which is a class of vertebral diseases, marked by pain, inflammation, and immobility of the spine and the adjoining, structures (ligaments and tendons). Spondylitis that involves multiple vertebral joints is known as spondylarthritis. In many cases, the sacroiliac joint, that connects the spine with the pelvis also becomes inflamed. Some of the neighboring joints such as that of the shoulders, ribs, knees, hips and often, the lower extremities are also affected. The places where the ligaments and the tendons attach to the bones also suffer inflammation. The patients typically experience mild to moderate back pain which is intermittent in nature. In the more advanced stages, a fusion of the affected bones occurs, leading to the loss of flexibility of the bones, stiffening of the rib cage and a subsequent reduction in lung capacity.
Are some people at greater risks for spondylitis?
The onset of the disease begins in the adolescence itself. The symptoms manifest themselves in a full-fledged manner before the age of 30. Nearly 5% of the patients develop the symptoms after the age of 45. In a majority of the cases, men are twice as likely to get the disease compared to women.
What are the main causes of spondylitis?
Spondylitis is triggered by environmental and genetic factors. Some of the causative factors are listed below-
- Natural disintegration and weakening of body muscles and joints occur with age (above 40) which can lead to joint damage
- Increased pressure on the vertebra due to obesity and overweight conditions
- Injury of the joints due to mechanical blow or rigorous physical activities
- Injured meniscus, tendons or ligaments due to accidental twisting and bending
- Ancestral history of osteoarthritis or spondylitis (due to HLA-DRB1 gene or mutation of collagen II gene)
- Existing joint diseases such as gout, rheumatoid arthritis or septic arthritis
- Lifting of heavy weights on a regular basis due to occupational requirements
- Autoimmune disorders leading to degeneration of the synovial tissues (primary contributor- Protein Tyrosine Phosphatase 22 gene)
- Food materials like artificial fats, processed meat, refined carbohydrates, alcohol that evoke inflammation
- Poor body postures
Genetics of spondylitis
 The genetics of the disease needs to be discussed separately since it plays a pivotal role in the occurrence of the disease in the future generations. The primary gene that is responsible for the disease is HLA-B27. It is not necessary that people who have this gene are definitely going to have spondylitis. The statistics of the National Institute of Arthritis and Musculoskeletal and skin diseases show that around 1 in 20 people who are the carriers of the HLA-B27 gene have the disease. The interaction between the CD8 T cells and HLA-B is believed to be the contributing factor in these cases. Recent studies have proven the roles of two additional genes- ERAP1 and IL23R in spondylitis.
The genetics of the disease needs to be discussed separately since it plays a pivotal role in the occurrence of the disease in the future generations. The primary gene that is responsible for the disease is HLA-B27. It is not necessary that people who have this gene are definitely going to have spondylitis. The statistics of the National Institute of Arthritis and Musculoskeletal and skin diseases show that around 1 in 20 people who are the carriers of the HLA-B27 gene have the disease. The interaction between the CD8 T cells and HLA-B is believed to be the contributing factor in these cases. Recent studies have proven the roles of two additional genes- ERAP1 and IL23R in spondylitis.
How do you know if a person has spondylitis?
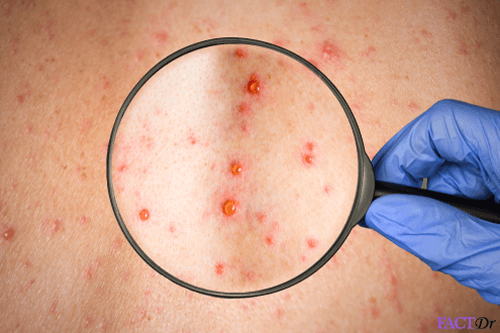
Spondylitis is an inflammatory disease marked by pain and stiffness of the spine. The following signs are readily identifiable-
- Temporary immobility and stiffness in the joints especially in the morning
- Pain and stiffness in the neck, back, and buttocks
- Pain and inflammation in the tendons and the ligaments, which is felt mainly in the chest, back of the heel or underneath the foot
- Inflammation and swelling of the joints and the soft tissues
- Joint pain during slight movements
- Temporary immobility (permanent immobility may also occur due to ankylosed or fused joints)
- Cracking and crunching sounds during normal joint movements
- Weakness and fatigue of muscles (may lead to muscular dystrophy)
- Pain radiating to neighboring regions (lower extremities)
- Redness around the joint area
- Extreme tenderness and touch sensitivity of joints
- Throbbing pain in the joint and muscles after some activity
- Bone and joint deformities (at an advanced stage)
- Disturbed sleep due to increased joint pain at night
- Difficulty maintaining normal body postures
- Difficulty performing mundane activities such as walking, running, climbing stairs
- Body aches and fever
- Extreme fatigue
- Loss of appetite
- Visible bulges (due to bone spurs)
What are the different types of spondylitis?
Based on the etiology spondylitis is of two types-
- Ankylosing spondylitis: It is a degenerative disease of the spine, characterized by an inflammation of the soft tissues surrounding the vertebral bones. It is characterized by pain and inflammation in the spine or the vertebra.
- Pott’s disease: In this disease, swelling and inflammation of the vertebral bones occur due to a form of tuberculosis that affects the lungs. The upper lumbar and the lower thoracic vertebra are mainly affected in this case.
Diagnostic tests
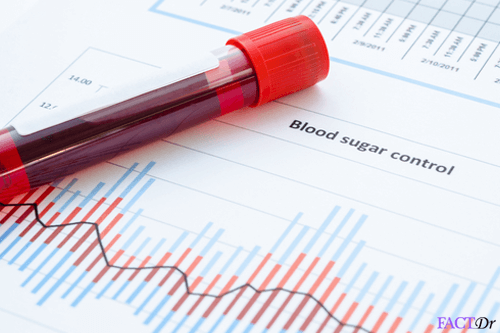
- Blood tests: The patients generally show an elevated level of C-reactive protein (CRP) and ESR.
- Genetic tests: These are required to test for HLA-B27.
- BASDAI: The Bath Ankylosing Spondylitis Disease Activity Index (BASDAI) gives a measure of the inflammatory burden of the existing diseases.
- Schober’s test: It measures the flexion of the lumbar spine.
Treatment and prevention
 The treatment of spondylitis focuses on decreasing the pain and stiffness and slowing down the spinal deformities. The medication usually comprises of NSAIDs (non-steroidal anti-inflammatory drugs), though an overdose of these could lead to severe gastrointestinal complications. An early diagnosis is important for effective recovery. Physiotherapy can also be prescribed in addition to the medications.
The treatment of spondylitis focuses on decreasing the pain and stiffness and slowing down the spinal deformities. The medication usually comprises of NSAIDs (non-steroidal anti-inflammatory drugs), though an overdose of these could lead to severe gastrointestinal complications. An early diagnosis is important for effective recovery. Physiotherapy can also be prescribed in addition to the medications.
Care should be taken while treating the patients with some of the broad-spectrum drugs such as corticosteroids. Otherwise additional systemic complications like cardiac and renal diseases may arise, which would worsen the pre-existing conditions.
In order to prevent the onset of spondylitis, one must be involved in regular physical exercises. More so, if he/she has a family history of spondylitis. Practice good posture and completely cut down on smoking and other forms of tobacco consumption. Consume a well-balanced nutritious diet and try to get ample of vitamin D and calcium.
- https://medlineplus.gov/ankylosingspondylitis.html
- https://www.niams.nih.gov/health-topics/ankylosing-spondylitis
- https://www.spondylitis.org/Ankylosing-Spondylitis
- https://www.mayoclinic.org/diseases-conditions/ankylosing-spondylitis/symptoms-causes/syc-20354808
- http://www.janssen.com/sites/www_janssen_com_australia/files/understanding_ankylosing_spondylitis_booklet.pdf
Dos and Don'ts
- A thin pillow and hard-mattress combination should be used. Wearing a cervical collar also helps.
- Lying flat on the stomach is not advisable. Avoid long drives and journeys. When traveling use the seat-belt to avoid jerking motion of the neck and spine.
- Perform high intensity and high impact exercises if suffering from cervical spondylitis.
- Sit stationary at one position for a long time. Take breaks from work/driving and move around a bit.
- Lift heavy weights. Also, avoid leaning your neck on one side while talking on the phone.
Help Others Be Fit
Related Conditions
Trending Topics